Why the future of surgery training could start with a VR headset
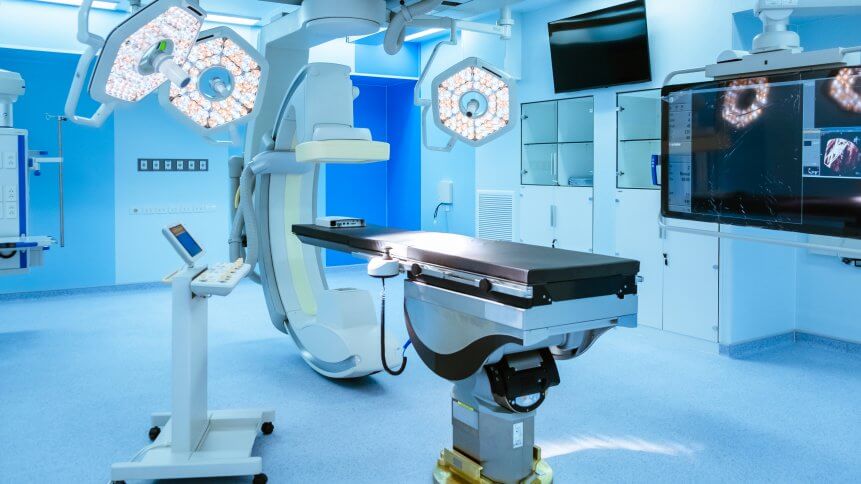
- Immersive technology can be used for drug development and surgical training
- Global coronavirus pandemic serves as a turning point for the adoption of VR in healthcare
- VR presents new ‘views’ and perspectives for surgeons teaching and learning medical procedures
The use of futuristic technology in the healthcare industry has surged in the past decade. Today, artificial intelligence (AI) is being used for diagnosis, drug design and development; medical supplies are being delivered by drone, and patients can have a consultation from their couch with video-conferencing software.
But in this ‘life-or-death’ industry, there is still plenty of room for innovation to change the status quo – to save time, money and, ultimately, lives.
Traditionally, surgical training involves a group of trainee specialists observing a surgical operation from a crowded operating theater in order to gain the necessary confidence to one day conduct the procedure themselves. For hundreds of years, surgeons have trained in the same way. They will travel, often hundreds of miles, to a physical location where an experienced surgeon will demonstrate a certain device or procedure. The trainees will observe and ask questions, and listen to commentary from their superiors and colleagues.
And while this approach works – it’s tried and tested – one company believes there’s a way of making the process more efficient.
Immertec is a software company that aims to elevate the surgical training experience by offering an opportunity for surgeons to train remotely in real-time using immersive virtual reality technology.
“VR is a new opportunity to disseminate knowledge and experience,” Erik Maltais, CEO of Immertec, told TechHQ.
The ultimate goal in surgical training is to build confidence and for trainee surgeons to be able to carry out the same surgical procedure independently. In order to achieve that level of confidence, the “golden standard” of training for a position is mentorship from an expert to an apprentice, Maltais said.
“However, as the volume of information increases, the volume of procedures, medical devices, and the number of surgeons have not increased at the same speed.” This discordant pace leads to inefficiencies that can incur large expenses and delays to training schedules.
Immertech’s aim is to ‘dissolve’ the physical barriers that restrict the adoption of modern medical devices and procedures.
Using Immertec’s virtual surgical training platform Medoptic, surgeons virtually scrub into an operating room with a VR headset from the comfort of their offices and homes, to consider adopting innovative procedures and devices.
“The benefit of virtual reality is that you could provide that experience as if someone’s present,” said Maltais, meaning trainees and mentors don’t always need to be flown around the world or country on overnight trips just to learn one procedure, and risk infection with operating rooms and healthcare facilities.
“Physicians sign up on our app to learn innovative procedures, they schedule training, and once approved, we mail them headsets. At the time of the surgery, they receive a secure code to log into the live operating room, via their headset,” said Maltais.
With a camera live-streaming from the operating room, trainees can look around the the environment as the surgeon works, while a moderator can overlay various other feeds, such as the view from an endoscopy: “They’re able to manipulate the overlay into a perfect spot, so the trainee can focus on what the surgeon’s doing or what the scrub nurse is doing, while still seeing what’s happening inside the patient for that specific portion of the procedure,” Maltais explained.
“There’s so much benefit to bringing in a world expert to help a surgeon without risking infection, or just having to travel and get on a plane,” said Maltais.
For Maltais, the benefits of using VR in surgical training aren’t just in making training more accessible and convenient to trainees, but to also reduce the burden on already over-stretched surgeons. The introduction of VR enables mentors to “do the training for the two hours that really matter and then right after that they can get back to their families and patients.”
Given the ability to access healthcare sites remotely, unsurprisingly, Maltais reports a surge of interest in Immertec’s solutions since the pandemic hit. But COVID-19, he adds, has only served as a catalyst to the healthcare industry’s adoption of these kinds of remote technologies as potential solutions to redistributing the burden on hospitals and staff.
“Before the pandemic, there were issues with foot traffic in the hospital,” Maltais said. “They wanted to decrease the traffic as much as possible because of burdens on the healthcare system.”
But with vigorous COVID-19 testing and mandatory 14-days quarantines in place, the new norm makes it even more challenging for expert specialists and trainee surgeons to continue to keep up their routine of surgical training. This is where VR comes into play as a possible solution, with Maltais referring to the pandemic as an “inflection point” for immersive technology in healthcare.
Alongside offering solutions for surgical training to continue uninterrupted, VR surgical training also reduces the need for personal protective equipment (PPE), meaning lowered costs and wastage.
In this sense, immersive technology like VR is transitioning from a “nice to have” experimental tool, to one that brings real positive impact and more fluidity to workflow. In a similar vein, doctors at a UK hospital have been using mixed reality headsets to help minimize infection as they treat patients with the coronavirus.
Microsoft Hololens headsets were worn by doctors to stream secure feeds of consultations to nearby rooms, allowing healthcare teams to see everything the wearer sees and feed back information, while the wearer can use gaze or voice control to view other data in front of their eyes, without contact.
As a result of this use, these doctors were ready to embrace the technology for new applications, including training, after the pandemic subsided.
YOU MIGHT LIKE

Rolls-Royce is training aerospace engineers with VR
Asked whether 5G will have a major impact on advancing the technology and its applications further, Maltais pointed to the possible decade-long timeframe for 5G’s full rollout. Instead, Immertech’s technology is designed so it can operate even without 5G-backed capabilities, and can still provide quality overlays and simulations by highlighting significant ‘moving elements’ of an environment, not every moving detail.
“Technology is built so that you don’t need 5G. We can actually ‘remote’ the people, the feed, the multiple overlay screens with the same internet that Netflix requires,” the CEO told us.
The main purpose of immersive technology is to lower the investments in terms of time, risks, and costs that come when surgeons may decide to adopt a piece of medical equipment or learn a medical procedure from expert surgeons aboard.
Will VR replace in-person surgical visitation?
“Absolutely not,” said Maltais.
“I think there’s some level of [in-person surgical visitation] that’s required. But, I do see VR as a way to provide access to innovation at a much faster rate with less risk.”